Tuesday, 7 April, 2026
Some conditions build slowly. You get time to think, maybe even ignore it for a day or two.
Meningitis doesn’t always work like that.
It can start off in a way that feels almost too familiar, fever, headache, a bit of fatigue. The kind of thing most of us have brushed aside at some point. And honestly, in many cases, it is something minor.
But occasionally, and this is where the concern lies, it isn’t.
Doctors tend to take meningitis seriously not because it’s always severe, but because when it is, it tends to move quickly. Faster than people expect.
What Is Meningitis?
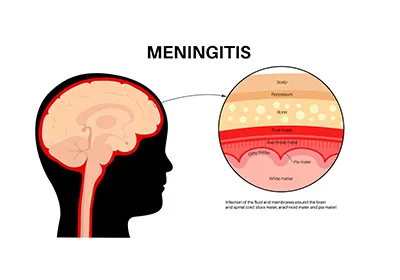
At a basic level, meningitis is inflammation of the meninges. These are the thin layers that cover the brain and spinal cord.
Now, inflammation anywhere in the body is usually manageable. But inside the skull, space is limited. Even a small amount of swelling can start to interfere with how the brain functions.
Infections are the usual cause. Viruses are common. Bacteria—less common, but more aggressive. Then there are outliers like fungal infections or immune-related causes, which don’t come up as often but still matter.
What throws people off, I think, is how ordinary it can feel in the beginning. There’s rarely a dramatic “start.”
Types of Meningitis
You’ll often hear doctors separate meningitis into categories. It might sound technical, but it’s actually quite practical—because each type behaves differently.
Bacterial Meningitis
bacterial meningitis is the one that tends to worry clinicians the most.
It can escalate in a matter of hours. Not always, but often enough that treatment usually begins before confirmation.
The bacteria involved—like Streptococcus pneumoniae or Neisseria meningitidis—are known to cause serious illness. That said, outcomes improve significantly when treatment starts early. Timing matters here more than anything else.
Viral Meningitis
Viral meningitis is more common and, in many cases, less severe.
People usually recover with rest, fluids, and some patience. But early on, it doesn’t look all that different from bacterial meningitis. That overlap creates a bit of uncertainty—which is why doctors don’t rely on assumptions.
You’ll often hear: “Let’s rule out the serious causes first.”
Fungal Meningitis
This type is rare. When it does appear, it’s usually in individuals with weakened immune systems.
It doesn’t spread person-to-person in the same way, so it tends to stay out of mainstream conversations. Still, in the right context, it becomes relevant quickly.
Non-Infectious Meningitis
Sometimes, there’s no infection at all.
Autoimmune conditions, certain cancers, or even medications can trigger inflammation. It’s less common, but it complicates diagnosis—especially in the early phase when symptoms don’t point clearly in one direction.
Warning Signs and Symptoms of Meningitis
This is probably the section people look for first—and understandably so.
Recognising meningitis symptoms isn’t always straightforward. In fact, many cases don’t present “by the book.”
You might notice:
- Fever that comes on suddenly
- A headache that feels… different (people often describe it that way)
- Neck stiffness
- Sensitivity to light
- Nausea, sometimes vomiting
- Confusion or difficulty focusing
And in more severe cases, seizures.
What’s tricky is that these symptoms don’t always appear together. Sometimes it’s just two signs that seem slightly off.
Classic Triad: Fever, Neck Stiffness, Photophobia
There’s something called the “classic triad”—fever, neck stiffness, and light sensitivity.
If all three show up, it raises concern quickly.
But here’s where it gets a bit less straightforward: many patients don’t have all three. So the absence of one doesn’t really reassure doctors as much as you might expect.
Meningitis Rash: The Glass Test
A meningitis rash can appear in certain cases, especially with meningococcal infections.
It looks like small red or purple spots. The detail that matters—these spots don’t fade when you press a glass against them.
It’s a simple check, but it’s often mentioned for a reason. If that rash appears alongside fever, it’s treated as urgent.
Symptoms in Infants and Young Children
With meningitis in children, things are less clear-cut.
Infants can’t describe what they’re feeling, so the signs tend to be behavioural:
- Constant or high-pitched crying
- A bulging soft spot on the head
- Difficulty feeding
- Vomiting
- Either unusual sleepiness… or the opposite—irritability
Parents often say, “Something just didn’t feel right.” That observation, while vague, is often valuable.
What Causes Meningitis?
When people look into the causes of meningitis, they’re usually expecting a single answer. It’s rarely that simple.
It could be:
- Bacterial infections spread through droplets
- Viral infections (quite common, actually)
- Fungal infections in specific high-risk groups
- Non-infectious triggers like immune reactions
Settings with close contact—schools, hostels—can increase exposure. That part is fairly well established.
Who Is Most at Risk?
Meningitis doesn’t affect everyone equally.
Some groups tend to be more vulnerable:
- Infants and young children
- Teenagers and college students in shared spaces
- Older adults
- People with weakened immune systems
- Those who haven’t received recommended vaccinations
In many situations, though, it’s not just about risk—it’s about response time after symptoms begin.
How Is Meningitis Diagnosed?
A reliable meningitis diagnosis usually needs more than observation.
Lumbar Puncture (Spinal Tap)
This is the key test.
A small sample of cerebrospinal fluid is taken from the lower back and analysed. It helps determine the cause—bacterial, viral, or otherwise.
It sounds intimidating. In practice, it’s a routine procedure in this setting and often essential.
Imaging and Blood Tests
Scans like CT or MRI may be done, especially if there’s concern about pressure in the brain.
Blood tests can help identify infection markers and sometimes the organism.
In reality, doctors often start treatment before everything is confirmed. Waiting isn’t always the safer option.
Treatment of Meningitis
Treatment depends on the cause, but timing is where things really matter.
Bacterial Meningitis Treatment
Bacterial meningitis requires immediate care.
Antibiotics are started as early as possible, often before confirmation. Once lab results come in, treatment may be refined.
Steroids are sometimes added to reduce inflammation.
This is where meningitis treatment becomes urgent, not something to delay.
Viral Meningitis Treatment
Treatment is usually supportive:
- Rest
- Fluids
- Pain relief
Antivirals are used in certain cases, though not always necessary.
Most people recover well—but early evaluation is still important.
ICU and Supportive Care
Severe cases may need intensive care.
Support might include oxygen, IV fluids, and monitoring for complications like seizures.
The focus is stability while treatment does its job.
Complications of Untreated Meningitis
Without timely treatment, complications can develop:
- Hearing loss
- Memory problems
- Seizures
- Brain injury
- Difficulties with coordination
What’s notable is how often early treatment reduces these risks.
Prevention: Vaccination and Hygiene
Prevention isn’t absolute, but it’s meaningful.
The meningitis vaccine protects against several serious bacterial strains.
Basic hygiene helps too—handwashing, avoiding close contact when someone is unwell, not sharing personal items.
Still, vaccination remains the most reliable protection.
Conclusion
Meningitis doesn’t always look alarming at first. That’s part of what makes it difficult.
If symptoms feel unusual—or seem to shift quickly—it’s worth getting checked. It may turn out to be nothing serious.
But if it isn’t, acting early can change the outcome in ways that are hard to overstate.
FAQs
Q1: How quickly does meningitis develop?
It can develop within hours, particularly in bacterial cases. Symptoms may start mild and worsen rapidly on the same day.
Q2: Is meningitis contagious?
Some forms, especially bacterial and viral meningitis, spread through respiratory droplets. Not all types are contagious.
Q3: How do I know if a rash is meningitis?
A meningitis rash does not fade when pressed with a glass. If it appears with fever or other meningitis symptoms, seek immediate care.
Q4: Can meningitis be treated at home?
No. It requires medical evaluation and often hospital treatment. Delays can be dangerous.
Q5: Is there a vaccine for meningitis?
Yes, the meningitis vaccine protects against several major bacterial strains and is recommended for many groups.


 Neurosciences
Neurosciences Bariatric Surgery
Bariatric Surgery